See some of the latest developments, discoveries and commentaries from the Washington University Department of Obstetrics and Gynecology.
For more news and updates:
Follow us on Twitter »
Listen to our Podcast »
Subscribe to our newsletter »
Media contact:
Diane Duke Williams
Associate Director for Media Relations
williamsdia@wustl.edu | 314-286-0111
Education team visits WUSM fair
The Education team got together on the WUSM campus to meet medical students and educate them on what WashU ObGyn is all about! The team included coordinators Kim Coombs & Rayna Mittler, Dr. Tammy Sonn, and Education Manager, Elizabeth Wanken.
Dickson, Khabele, Longmore elected to Association of American Physicians (Links to an external site)
Three physician-scientists at Washington University School of Medicine in St. Louis have been newly elected to the Association of American Physicians. Membership in the organization is an honor bestowed on physicians who lead innovative scientific research to improve health care. Khabele, the Mitchell & Elaine Yanow Professor and head of the Department of Obstetrics & Gynecology, […]
Dr. Whorton and Dr. Sharifi awarded Accolade
Residents Dr. Allison Whorton and Dr. Mitra Sharifi were awarded an accolade for contributing to a positive learning environment. Both awards were reported under WashU’s Med’s SAFE reporting. Washington University School of Medicine strives to maintain an environment conducive to learning, research, and high-quality patient care. We aspire to an environment that is inclusive and […]
Black Maternal Health Week 2024
We are excited to invite you to participate in the upcoming events for Black Maternal Health Week, which runs from April 11-17, 2024. This week provides an opportunity for us to raise awareness and take action to improve the health and well-being of Black mothers and birthing people. As part of our commitment to supporting […]
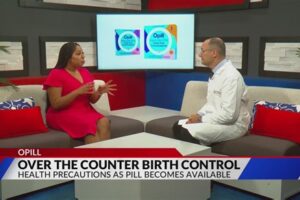
Dr. Eisenberg on Fox2 on the first daily contraceptive pill for over-the-counter purchase
“The FDA has approved the first daily contraceptive pill for over-the-counter sale, enhancing access to pregnancy prevention options. Dr. David Eisenberg, Chief Division of Complex Family Planning at Washington University and Barnes-Jewish Hospital, talks about new developments in over-the-counter birth control. Dr. Eisenberg says that the pill, containing an ingredient used in birth control since […]